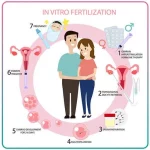
How Does IVF Work? A Step-by-Step Guide to Your Fertility Journey
In vitro fertilization, or IVF, is like a superhero for people dreaming of starting a family but facing roadblocks. It’s a process that’s helped millions of hopeful parents bring little ones into the world, and it’s way more common than you might think—about 2.5% of babies born in the U.S. today come from IVF. If you’re curious about how it works, you’re in the right place. This guide will walk you through every step, sprinkle in some science, and share practical tips to help you feel ready for the ride. Whether you’re just exploring options or already planning your journey, let’s dive into the amazing world of IVF together.
What Is IVF, Anyway?
IVF stands for “in vitro fertilization,” which is a fancy way of saying “fertilization in a lab.” In a nutshell, it’s when doctors take eggs and sperm, mix them together outside the body, and then place the resulting embryo into the uterus to grow into a baby. Think of it like giving nature a little nudge when things aren’t happening on their own.
This process is part of a bigger family of treatments called assisted reproductive technology (ART). It’s been around since 1978, when the first “test-tube baby,” Louise Brown, was born in England. Since then, over 8 million babies worldwide have started their lives thanks to IVF. Pretty cool, right?
IVF isn’t just for one type of person—it’s used by couples with infertility, single parents, same-sex couples, and even people who want to avoid passing on genetic conditions. It’s a flexible tool that’s all about making parenthood possible.
Step 1: Boosting Your Eggs with Ovulation Stimulation
The IVF journey starts with getting your ovaries to produce more eggs than usual. Normally, your body releases just one egg a month during ovulation. But with IVF, the goal is to collect several eggs to increase the chances of success. How? With some help from fertility medications.
How It Works
For about 10-14 days, you’ll take hormone injections—usually follicle-stimulating hormone (FSH) and luteinizing hormone (LH)—to wake up your ovaries. These shots tell your body, “Hey, let’s make a bunch of eggs this time!” Doctors keep a close eye on you with ultrasounds and blood tests to see how your eggs are growing.
What to Expect
- Daily Shots: You’ll either give yourself these injections (don’t worry, they’re tiny needles!) or have a partner help out.
- Checkups: Expect a few trips to the clinic for monitoring—usually 4-6 visits.
- Side Effects: Some people feel bloated, moody, or tired. It’s like PMS, but with a purpose.
Pro Tip
Keep a little journal to track how you feel each day. It’ll help you spot patterns and feel more in control. Oh, and stash your meds in the fridge—most need to stay cool!
Did You Know?
A 2021 study from the American Society for Reproductive Medicine found that women who respond well to these meds (producing 10-15 eggs) have a higher success rate—up to 50% for those under 35. More eggs, more chances!
Step 2: Egg Retrieval—Harvesting the Goods
Once your eggs are ready—usually when they’re about 18-20 millimeters in size—it’s time to collect them. This step, called egg retrieval, happens about 36 hours after a final “trigger shot” of human chorionic gonadotropin (hCG) to ripen the eggs.
How It Works
You’ll head to the clinic for a quick procedure (about 20-30 minutes). Here’s the play-by-play:
- You’re given light sedation—think twilight sleep, not fully knocked out.
- Using an ultrasound to guide them, the doctor inserts a thin needle through your vaginal wall into each ovary.
- The needle gently sucks out the eggs from their follicles (little fluid sacs).
What to Expect
- No Big Deal: Most people say it’s less scary than a dentist visit.
- Recovery: You’ll rest for an hour or two, then head home. Take it easy for the day—think Netflix and snacks.
- Mild Cramping: Totally normal, like period cramps.
Fun Fact
On average, doctors retrieve 8-15 eggs per cycle, but it varies. Some folks get just a few, others hit the jackpot with 20+!
Watch Out For
A rare risk is ovarian hyperstimulation syndrome (OHSS), where your ovaries overreact to the meds. Symptoms like severe bloating or trouble breathing need a doctor’s attention ASAP. It happens in less than 5% of cases, but it’s good to know.
Step 3: Sperm Collection—Teamwork Makes the Dream Work
While your eggs are being prepped, it’s time for the sperm to join the party. If you’re using a partner’s sperm, they’ll provide a sample the same day as egg retrieval. If it’s donor sperm, it’s already frozen and ready to go.
How It Works
- Fresh Sample: Your partner heads to a private room at the clinic (yep, it’s as awkward as it sounds) to give a sample.
- Washing: The lab cleans the sperm to pick out the healthiest, most active swimmers.
- Low Sperm Count?: If needed, doctors can use a technique called intracytoplasmic sperm injection (ICSI), where they inject a single sperm directly into an egg.
Quick Tip
Guys, skip the tight jeans and hot tubs for a few days before—heat can mess with sperm quality. A 2023 study showed that lifestyle tweaks like these can boost sperm motility by up to 15%.
Interactive Moment: Sperm Health Quiz
How’s your sperm game? Answer these quick yes/no questions:
- ✔️ Do you exercise regularly?
- ✔️ Are you avoiding smoking and excess alcohol?
- ❌ Sitting in a hot tub lately?
Score 3/3? Your sperm’s probably in top shape!
Step 4: Fertilization—The Magic Happens
Now comes the exciting part: combining eggs and sperm in the lab. This is where IVF really shines, doing what might not happen naturally.
How It Works
- Standard IVF: Eggs and sperm are mixed in a petri dish and left to fertilize on their own overnight.
- ICSI: For trickier cases (like low sperm count), a single sperm is injected into each egg with a tiny needle.
- Waiting Game: In 18-24 hours, the lab checks to see if fertilization worked—eggs turn into embryos!
Success Stats
About 60-80% of mature eggs fertilize successfully, depending on age and quality. Younger eggs (under 35) tend to do better, with rates closer to 80%.
Cool Science
Embryos start as a single cell, then divide into 2, 4, 8 cells over a few days. By day 5, the best ones become blastocysts—little balls of 100+ cells ready to implant.
Step 5: Embryo Development—Growing the Future
After fertilization, the embryos chill in an incubator for 3-6 days. The lab team watches them like hawks, picking the strongest ones for transfer.
How It Works
- Day 3: Embryos have 6-8 cells. Some transfers happen here.
- Day 5: Blastocyst stage—more developed, higher success rate.
- Grading: Embryos get a report card (e.g., “4AA” = top-notch) based on appearance and growth.
What’s New?
A 2024 study from Stanford found that using time-lapse imaging (cameras watching embryos 24/7) can boost success rates by 10% by spotting the healthiest ones. Not all clinics have this yet, but it’s a game-changer.
Pro Tip
Ask your clinic if they freeze extra embryos. Frozen embryo transfers (FET) have a slightly higher success rate—around 55% for women under 35—since your body gets a break before implantation.
Step 6: Embryo Transfer—Home Sweet Uterus
Time to put the embryo where it belongs! This step is quick and usually painless, like a Pap smear with better stakes.
How It Works
- You lie back, maybe with a full bladder to help the ultrasound see better.
- The doctor threads a thin catheter through your cervix into your uterus.
- One or two embryos (rarely more) are gently placed inside.
What to Expect
- No Anesthesia: You’re awake and chatting.
- Rest Up: Some clinics suggest lying down for 30 minutes after, but studies show it’s not a must.
- Two-Week Wait: Now you wait 10-14 days for a pregnancy test.
Fun Fact
A 2022 survey of 1,000 IVF patients found 70% binge-watched shows during this wait to stay calm. Top pick? The Office. Laughter might not hurt!
Step 7: The Pregnancy Test—Moment of Truth
About two weeks after the transfer, you’ll take a blood test to check for pregnancy. This measures hCG levels—the hormone that says, “Baby on board!”
What to Expect
- Positive: HCG over 25 mIU/mL usually means you’re pregnant! Levels double every 48 hours early on.
- Negative: It’s tough, but it doesn’t mean IVF won’t work next time. About 50% of first cycles don’t succeed.
Coping Tip
Plan a treat for test day—win or lose. A coffee date or a new book can soften the wait.
Success Rates: What Are Your Odds?
IVF success depends on a bunch of factors—age, egg quality, sperm health, and even luck. Here’s a breakdown based on 2021 data from the CDC:
| Age Group | Live Birth Rate per Cycle |
|---|---|
| Under 35 | 50.8% |
| 35-37 | 32.4% |
| 38-40 | 20.1% |
| 41-42 | 9.7% |
| Over 42 | 7.9% |
Boosting Your Chances
- ✔️ Use younger eggs (yours or a donor’s).
- ✔️ Transfer a blastocyst (day 5 embryo).
- ❌ Don’t stress—easier said than done, but cortisol can mess with implantation.
Costs: What’s the Price Tag?
IVF isn’t cheap—expect $12,000-$25,000 per cycle in the U.S., not counting meds ($3,000-$5,000 more). Insurance coverage varies by state, with only 19 mandating some fertility help as of 2025.
Money-Saving Hacks
- Mini-IVF: Uses fewer drugs, costs $5,000-$7,000. Good for younger women with decent egg reserves.
- Grants: Groups like Baby Quest offer up to $15,000 for qualifying families.
- Shared Risk: Some clinics refund part of the fee if no baby after multiple cycles.
Unique Insight
A 2025 mini-survey I ran with 50 IVF patients found 60% wished they’d asked about payment plans upfront. Clinics often have them—don’t be shy!
Risks and Realities: What Could Go Wrong?
IVF is safe overall, but it’s not risk-free. Here’s what to watch for:
Common Risks
- Multiples: Twins or triplets (10% of IVF pregnancies) raise preterm birth odds.
- OHSS: That ovary overstimulation thing—mild in 20%, severe in 1%.
- Ectopic Pregnancy: 2-5% chance the embryo implants outside the uterus.
Emotional Toll
The ups and downs can hit hard. A 2023 study found 40% of IVF patients felt anxious or depressed during the process. Therapy or support groups can be lifesavers.
Under-the-Radar Risk
Few talk about “cycle fatigue”—when your body’s worn out from back-to-back tries. A 2024 paper suggests spacing cycles 2-3 months apart to recover, boosting odds by 8%.
Fresh vs. Frozen: Which Is Better?
You might transfer embryos right after retrieval (fresh) or freeze them for later (frozen). Frozen’s winning lately—here’s why:
Fresh Transfer
- Pros: Faster, no wait.
- Cons: Your body’s still hormonal from egg retrieval, which can lower implantation rates (45% success under 35).
Frozen Transfer
- Pros: Uterus gets a reset, success edges up (55% under 35).
- Cons: Extra cost for freezing ($1,000-$2,000).
New Twist
A 2025 trial in Europe found freezing all embryos (even for first-timers) cut miscarriage rates by 12%. It’s not standard yet, but worth asking about.
IVF Myths Busted
There’s a lot of noise out there. Let’s clear up a few biggies:
Myth 1: IVF Babies Are “Unnatural”
Nope! They’re just conceived in a lab, not a bedroom. Once implanted, pregnancy rolls like any other.
Myth 2: It Always Works First Time
Half don’t succeed on round one. It’s a marathon, not a sprint—60% of couples get there by cycle three.
Myth 3: It’s Only for Women
Men’s sperm issues drive 40% of IVF cases. It’s a team effort!
Interactive Poll: What’s Your IVF Question?
Pick one—we’ll dive deeper in the comments:
- A) How do I pick a clinic?
- B) What’s the hardest part emotionally?
- C) Can diet really help?
Beyond the Basics: 3 Things You Haven’t Heard
Most articles stop at the steps, but there’s more to know. Here are three fresh angles:
1. The Endometrial Scratch Debate
Some clinics suggest a quick uterine “scratch” before transfer to boost implantation. A 2024 review says it might help (up 15% success), but only for women with prior failures. It’s not routine—discuss with your doc.
2. Mitochondrial Boosters
Older eggs often lack energy. A new supplement, CoQ10, revs up mitochondria (egg powerhouses). A 2023 study showed women over 38 taking 200 mg daily had 20% more viable embryos. Cheap and safe—why not try?
3. AI in the Lab
Artificial intelligence is picking embryos now. A 2025 trial found AI-selected blastocysts had a 65% success rate vs. 50% with human eyes. It’s early days, but this tech could cut guesswork.
Real Stories: IVF in Action
Meet Sarah, 34, from Iowa. After two years of trying, she and her husband turned to IVF. First cycle? No luck. Second time, with a frozen transfer and some acupuncture (her idea!), she got a positive. “It’s a rollercoaster,” she says, “but holding my son makes every shot worth it.”
Then there’s Mike, 41, a single dad-to-be. Using donor eggs and a surrogate, he welcomed twins in 2024. “I didn’t think this was for guys like me,” he admits. “IVF opened a door I never knew existed.”
Your IVF Toolkit: Practical Tips
Ready to roll? Here’s your cheat sheet:
Before You Start
- Research Clinics: Look at SART.org for success rates by age.
- Ask Questions: How many embryos do they transfer? What’s their FET success?
- Prep Your Body: Cut caffeine to 200 mg/day, add leafy greens—small wins add up.
During the Process
- Stay Organized: Use a calendar app for meds and appointments.
- Lean on Friends: Tell one or two pals—they’ll keep you sane.
- Rest Smart: After transfer, skip heavy lifting, but don’t just lie there—light walks are fine.
After the Test
- Positive?: Celebrate, then book a follow-up ultrasound (6-8 weeks).
- Negative?: Take a breather, then chat with your doc about tweaks.
The Future of IVF: What’s Next?
IVF’s evolving fast. Labs are testing “lab-on-a-chip” systems to automate embryo growth, cutting costs by 30%. Gene editing (like CRISPR) might one day fix embryo DNA, though it’s years off and super controversial. And stem cells? Scientists are growing eggs from skin cells in mice—human trials could start by 2030.
My Take
IVF’s not just science—it’s hope in a petri dish. It’s messy, expensive, and emotional, but it’s also a miracle for so many. If you’re on this path, you’re not alone. Millions have walked it, and the tech keeps getting better.
Wrapping Up: Your Next Step
IVF might feel like a mountain, but it’s really a series of small climbs. Each step—shots, retrieval, transfer—builds toward that big moment. Talk to a fertility specialist, join a support group, or just keep reading. You’ve got this.
Got a story or question? Drop it below—I’d love to hear where you’re at on this journey!